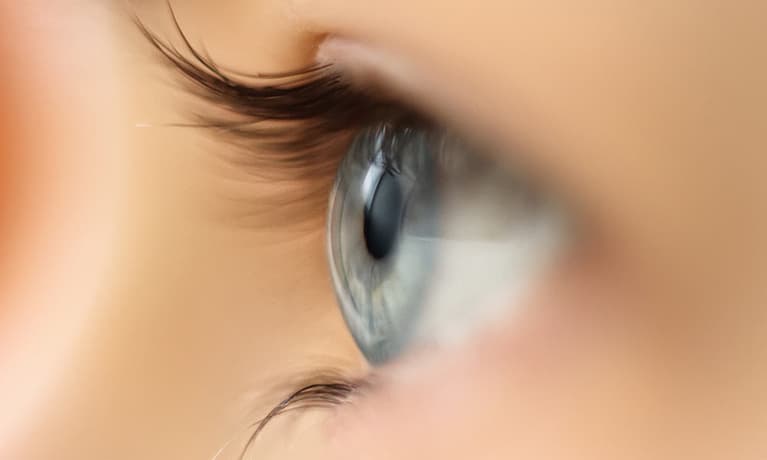
The cornea is the clear front surface of the eye; the part of the eye on which contact lenses are worn. For normal vision to occur, light rays must pass easily through the cornea, without distortion.
When the cornea is damaged, cloudy, or has an irregular curvature, clear vision is not possible. This is similar to a camera with scratches or fingerprints on the front of the lens, which would prevent that camera from taking clear pictures.
Corneal Transplants
When it is no longer possible to improve a patient’s vision to adequate levels with glasses or contact lenses because of corneal disease, a corneal transplant is often recommended.
This procedure is called a Penetrating Keratoplasty (PK) and involves removing the cloudy, diseased cornea and replacing it with clear corneal tissue from an organ donor. This is sometimes called a “full-thickness transplant” because all layers of the cornea are removed and replaced with healthy donor tissue. In some corneal disorders, only one layer of the cornea is unhealthy. Techniques that replace just the unhealthy layer of the cornea are evolving and are sometimes called “partial-thickness transplants.”
Who Needs A Corneal Transplant (PK)?
The types of patients that need full-thickness corneal transplants usually have scarring and opacification, swelling, or irregular curvature/astigmatism that is so extensive the only thing that will help them is a totally new cornea. For example, patients that have keratoconus, which can lead to extensive scarring and irregular astigmatism, may need a full-thickness transplant. Other reasons someone might need a full-thickness corneal transplant include trauma, bacterial or viral infections, and severe corneal swelling that eventually results in cloudiness.
What Are the Risks?
 Corneal transplants, like all surgeries, involve risks including infection and bleeding. They also carry some risk of rejection of the donated tissue, like all types of transplants. The donor tissue is sewn into place with fine sutures. Trauma after surgery, such as falling or getting hit in the eye, can result in opening of the wound. Astigmatism, which means a curvature that isn’t perfectly round and regular, is common after PK surgery. This astigmatism can be controlled by careful and selective suture removal. To see their best, some patients may need to wear a rigid gas permeable contact lens after their transplant to correct astigmatism. Transplants may also age and fail with time. It is important to remember that a transplant is a more involved surgery than cataract surgery and entails a much more prolonged post-operative course. When you have a transplant you will see your doctor many times for the year after your surgery as he/she works to improve your vision. It may take up to a year to achieve good, stable vision after this surgery.
Corneal transplants, like all surgeries, involve risks including infection and bleeding. They also carry some risk of rejection of the donated tissue, like all types of transplants. The donor tissue is sewn into place with fine sutures. Trauma after surgery, such as falling or getting hit in the eye, can result in opening of the wound. Astigmatism, which means a curvature that isn’t perfectly round and regular, is common after PK surgery. This astigmatism can be controlled by careful and selective suture removal. To see their best, some patients may need to wear a rigid gas permeable contact lens after their transplant to correct astigmatism. Transplants may also age and fail with time. It is important to remember that a transplant is a more involved surgery than cataract surgery and entails a much more prolonged post-operative course. When you have a transplant you will see your doctor many times for the year after your surgery as he/she works to improve your vision. It may take up to a year to achieve good, stable vision after this surgery.
Full-thickness corneal transplant surgery is a technically demanding procedure that requires a doctor who has had specialized training. It’s not a surgery that yields immediate results but has the potential to change a blind eye into an eye with excellent vision.
To schedule an appointment for a corneal evaluation with Dr. Edmonds, please call Milwaukee Eye Care at 414-271-2020.