Diabetic Eye Care
Approximately 16 million Americans have diabetes. Many patients living with this condition are unaware that diabetes may affect their eyes and can lead to sudden vision loss or permanent blindness. Each year 12,000 to 24,000 people lose their sight because of diabetes. Diabetic retinopathy is the leading cause of preventable blindness in the United States.
Patients with any form of diabetes are at risk, including Type 1 insulin-dependent diabetics, Type 2 non-insulin-dependent diabetics, and Type 2 insulin requiring diabetics.
Many patients with early stages of diabetic eye disease do not have any visual symptoms. We can only discover the early and most treatable forms of diabetic retinopathy during a complete eye exam.
What is Diabetic Retinopathy?
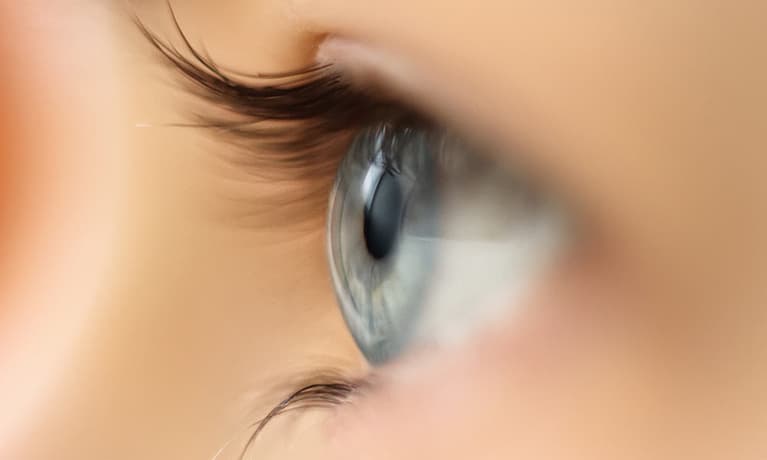
Diabetic retinopathy is a potentially vision-threatening condition in which the blood vessels in the retina (the area of light-sensitive cells that line the back of the eye) become damaged. These damaged vessels can then leak, causing swelling or hemorrhaging in the retina. In more advanced cases, abnormal new blood vessels grow on the surface of the retina. These can cause large hemorrhages in the eye and/or retinal detachment. The longer you have diabetes, the greater your chance of developing diabetic retinopathy. Over one-third of those diagnosed with diabetes don’t get the recommended vision care.
Recommended Care
If we diagnose you with any form of diabetes (insulin requiring or not), it is essential that you have a complete dilated eye exam at least once a year. During this exam, the eye doctor will use eye drops to painlessly and temporarily widen the pupil to make it easier to see inside your eyes and examine your retina. Your eye doctor will recommend more frequent examinations if they detect problems.
Women with diabetes should have an eye exam if they are planning to become pregnant, early in the first trimester, and every one to three months during pregnancy. This is because diabetic retinopathy can progress rapidly during pregnancy.
Recent studies show that controlling diabetes by self-monitoring blood sugar levels, and taking oral medication or insulin injections, can prevent or slow the development of diabetic retinopathy and other complications of diabetes. Early diagnosis of diabetes and controlling blood sugar levels and high blood pressure through diet, exercise and proper medication can help control eye diseases associated with diabetes.
Symptoms
There are no symptoms in the early stages of diabetic retinopathy. It may not affect your vision until the disease worsens. Treatment is often most effective if we do it before visual symptoms have developed.
You should see your eye doctor immediately if you experience:
- Blurred vision that lasts more than a few minutes
- Blurred vision that is not associated with a change in blood sugar
- Many small black spots in your field of vision
Treatment
An effective partnership between you, your primary care physician, and your eye doctor is necessary to make sure we provide proper eye care and treatment.
The standard treatment for diabetic retinopathy is laser photo-coagulation. This is done in several ways, depending on the retinopathy a patient has. Treatment is directed at leaking blood vessels near the center of the retina if “diabetic macular edema” is the problem. If more advanced retinopathy has developed and caused abnormal blood vessels to grow on the surface of the retina (also known as proliferative retinopathy), laser treatment is directed at the peripheral retina. Both laser treatments prove to greatly reduce the likelihood of vision loss from diabetes.
Where Can I Get More Information?
Your eye doctor is the best source of information on diabetic eye disease, as well as eye health and safety. To schedule an appointment call 414-271-2020.